Three quarters of Americans with health insurance coverage believe too many hurdles exist between patients and doctor-prescribed medicines
Washington, DC, July 12, 2021 — A new Ipsos poll finds that three quarters of Americans with some form of health insurance believe too many hurdles stand between patients and the medicines prescribed by their doctor, with nearly one in three patients having experienced utilization management restrictions on their prescription medicines, including formulary exclusions, prior authorizations, step edits, and high out-of-pocket costs.
52% of Americans with health insurance are concerned about how out-of-pocket costs may impact their ability to access prescription medicines while just under half report being concerned that the medicines they need are not covered by their insurance plan.
Overall, one in five adults covered by health insurance say that they failed to pick up a doctor-prescribed medication from the pharmacy in the past year. The two most common reasons for patients abandoning their prescriptions were an inability to afford out-of-pocket expenses (co-pays, deductibles, and coinsurance) and insurance plans not covering the medicine prescribed. Importantly, among those who did not fill a prescription, half said that their health suffered as a result, with one in four being prescribed more medication (26%) and/or ending up in the emergency room (23%).
Nine in ten (92%) Americans believe that doctors – not insurers – should make therapy decisions and 84% of those surveyed support the notion of having insurance policies for medicines evaluated for fairness by an independent, non-biased third party.
Detailed Findings
Two thirds of Americans with some form of health insurance coverage worry about their ability to access prescription medicines (67%). This is especially true for adults under the age of 35 (80% vs. 57% of those aged 55 and over), those in low-income households (74% of those with a household income less than $50,000 vs. 62% of those earning at least $100,000), and adults living in the South (72% vs. 59% of those living in the West).
- This includes one in two Americans (52%) who report being concerned with how out-of-pocket costs may impact their ability to access prescription medicines – especially adults under the age of 35 (62%), those in low-income households (59% of those with a household income less than $50,000), and adults in the Midwest (56%) and South (55%).
- Just under half also worry that lack of insurance coverage will hinder their ability to access prescription medicines (48%). Once again, young adults (58% of those aged 18-34) and those living in the South (54%) are considerably more likely to worry about this compared to their demographic counterparts.
- Getting authorization from their insurer before the cost of the medicine is reimbursed is a concern for more than two in five (43%). This figure jumps to at least 50% among young adults (54% of those aged 18-34), those in low income households (50%), those living in the South (50%), and non-White respondents (52%).
- Another 43% report being concerned with having to first try cheaper alternatives to the medicine prescribed before being allowed to receive the originally prescribed medicine. Here too, younger adults (54% of those aged 18-34), those in low income households (47%), those living in the South (47%), and non-White Americans (51%) are significantly more likely to report worrying about this.
- Fewer are concerned with lack of medicine availability, though more than a third worry about how this will impact their ability to access prescription medicines (35%). Adults under the age of 35 (46%) and those with a household income under $50,000 (44%) are particularly likely to report being concerned.
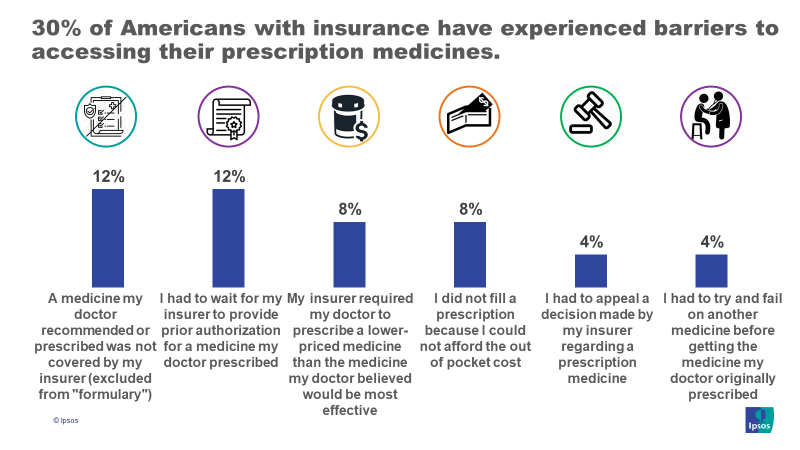
Three in ten have experienced issues accessing prescription medication in the past year – and this jumps to 45% among both parents with children at home and those between the ages of 18-34.
- This includes more than one in ten who say that a medicine recommended or prescribed by their physician was not covered by their insurer (12%) and another 12% who say they had to wait for their insurer to provide prior authorization for prescribed medicine.
- Other access issues experienced include not filling a prescription due to an inability to afford the out-of-pocket costs (8%) and the insurer requiring a doctor to prescribe a lower-priced medicine than the one believed to be most effective (8%).
One in five Americans (21%) say that they did NOT fill or pick up a prescription from the pharmacy that was prescribed to them (or someone in their household) by a doctor in the past year. Among those who did not fill or pick up a prescription, one in two (50%) say that their health suffered as a result of this.
- Not being able to afford the out-of-pocket cost before deductible (28%) or the co-pay (16%) were among the most common reasons mentioned for not filling or picking up a prescription. Another 19% say they were unable to fill a prescription because their insurance would not cover the medicine, rounding out the top three reasons.
- Those most vulnerable to suffering health consequences because they couldn’t fill their prescription include: younger adults (59% of those between the ages of 18-34) and non-White respondents (63%).
- Half of those whose health suffered say they needed to make another appointment with their physician (50%). One in four were prescribed more medications (26%) and/or ended up in the emergency room (23%).
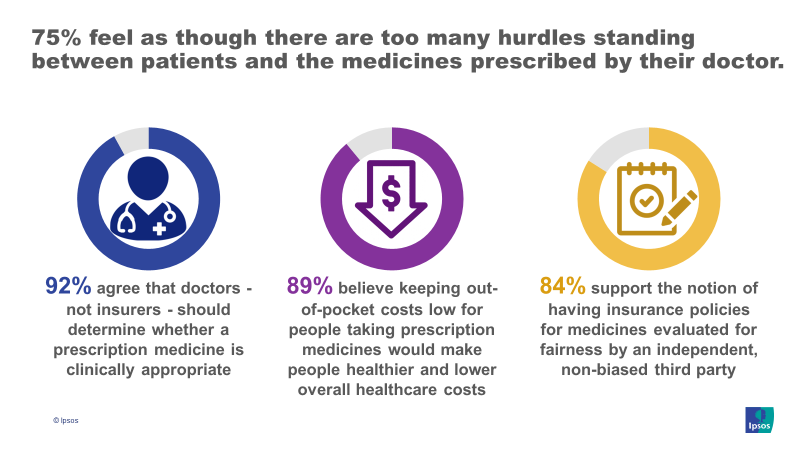 Three quarters of those with insurance coverage believe that too many hurdles stand between patients and the medicines prescribed by their doctor (75%). An even greater proportion agree that keeping out-of-pocket costs low for people taking prescription medicines would make people healthier and lower overall healthcare costs (89%).
Three quarters of those with insurance coverage believe that too many hurdles stand between patients and the medicines prescribed by their doctor (75%). An even greater proportion agree that keeping out-of-pocket costs low for people taking prescription medicines would make people healthier and lower overall healthcare costs (89%).
There is consensus among Americans that doctors - not insurers - should determine whether or not a prescription medicine is clinically appropriate (92%). Among all surveyed, 84% support having insurance policies for medicines evaluated for fairness by an independent, non-biased third party. 72% also believe drug manufacturers and private insurance companies should negotiate prices based on assessments made by independent third parties. Older adults are significantly more likely to agree with both statements.
About the Study
These are the findings from an Ipsos poll conducted May 11 - 13, 2021 on behalf of Novartis Pharmaceuticals Corporation and Reservoir Communications Group. For the survey, a sample of 1,122 adults ages 18 and over from the continental U.S., Alaska and Hawaii was interviewed online in English. To qualify for the survey, respondents had to be covered by some form of health insurance.
The sample for this study was randomly drawn from Ipsos’ online panel (see link for more info on “Access Panels and Recruitment”), partner online panel sources, and “river” sampling (see link for more info on the Ipsos “Ampario Overview” sample method) and does not rely on a population frame in the traditional sense. Ipsos uses fixed sample targets, unique to each study, in drawing a sample. After a sample has been obtained from the Ipsos panel, Ipsos calibrates respondent characteristics to be representative of the U.S. Population using standard procedures such as raking-ratio adjustments. The source of these population targets is U.S. Census 2018 American Community Survey data. The sample drawn for this study reflects fixed sample targets on demographics. Posthoc weights were made to the population characteristics on gender, age, race/ethnicity, region, and education.
Statistical margins of error are not applicable to online non-probability polls. All sample surveys and polls may be subject to other sources of error, including, but not limited to coverage error and measurement error. Where figures do not sum to 100, this is due to the effects of rounding. The precision of Ipsos online polls is measured using a credibility interval. In this case, the poll has a credibility interval of plus or minus 3.3 percentage points for all respondents. Ipsos calculates a design effect (DEFF) for each study based on the variation of the weights, following the formula of Kish (1965). This study had a credibility interval adjusted for design effect of the following (n=1,122, DEFF=1.5, adjusted Confidence Interval = +/-4.8 percentage points for all respondents).
For more information on this news release, please contact:
Marie-Pierre Lemay
Director, US
Public Affairs
[email protected]
About Ipsos
Ipsos is the world’s third largest market research company, present in 90 markets and employing more than 18,000 people.
Our passionately curious research professionals, analysts and scientists have built unique multi-specialist capabilities that provide true understanding and powerful insights into the actions, opinions and motivations of citizens, consumers, patients, customers or employees. We serve more than 5000 clients across the world with 75 business solutions.
Founded in France in 1975, Ipsos is listed on the Euronext Paris since July 1st, 1999. The company is part of the SBF 120 and the Mid-60 index and is eligible for the Deferred Settlement Service (SRD).
ISIN code FR0000073298, Reuters ISOS.PA, Bloomberg IPS:FP www.ipsos.com



