GP Patient Survey: Experiences of young patients (aged 16 – 24 years old)
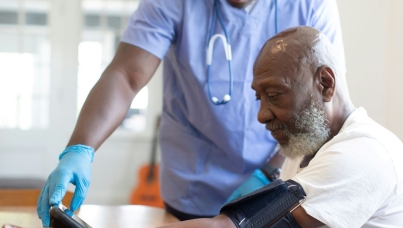
‘Young people’ is a common term used to describe those under the age of 25. Good health for young people is central to overall wellbeing, forming the foundation for good health in later life. Despite this, there is growing concern for young people’s health. For example, the Office for National Statistics have provided evidence which shows that the proportions of young people reporting symptoms of mental health issues such as anxiety and depression have been growing in recent years.
Heather Ashford looks at data from the 2018 GP Patient Survey (GPPS) and what the survey tells us about the experiences of young patients aged 16 – 24 years old, compared with the experiences of older patients (those aged 25 years and over).
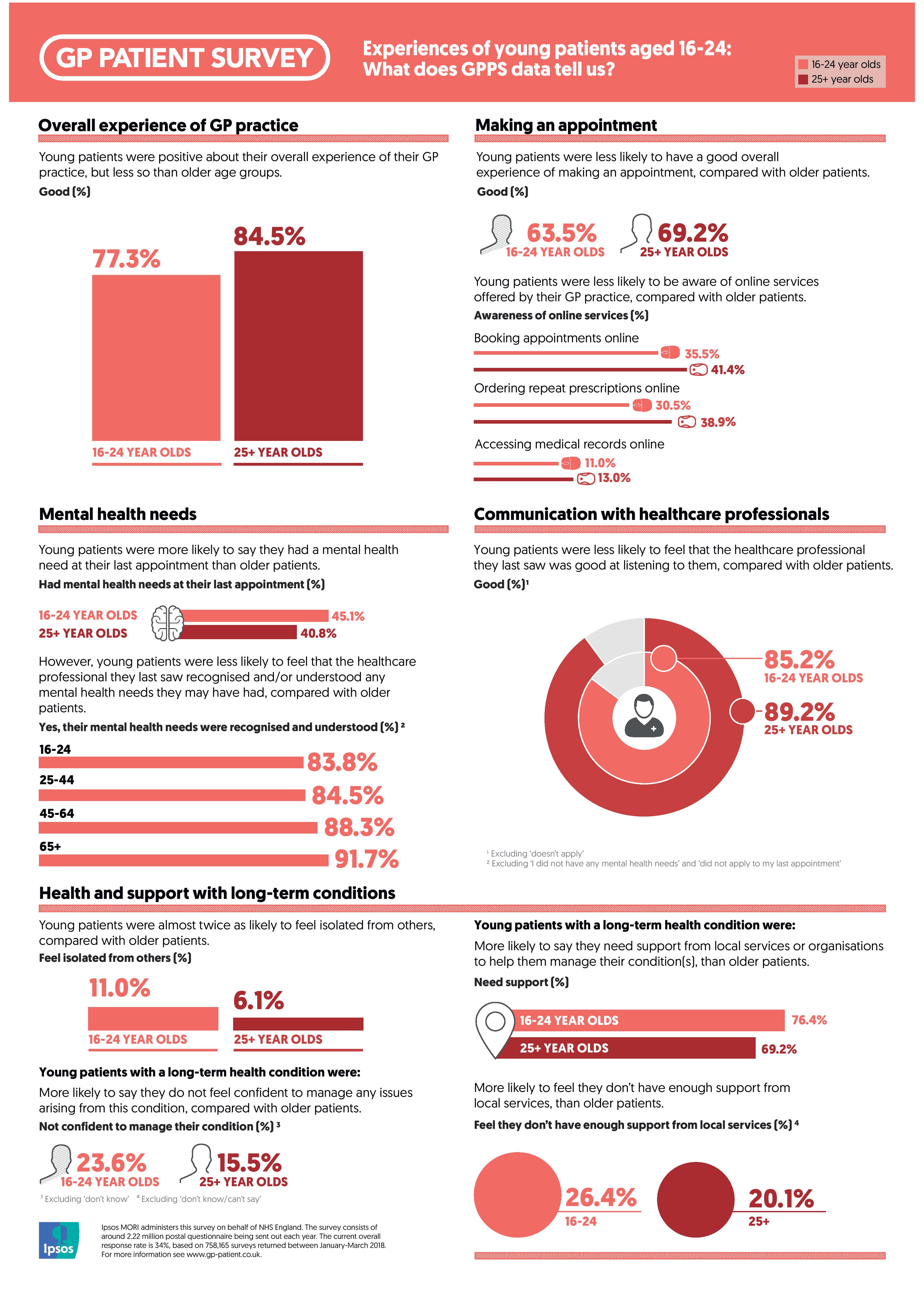
Around 37,000 people who answered the 2018 survey were aged 16 – 24. They were positive about their overall experience of their GP practice (77.3% of young patients said it was either very or fairly good) but less so than older patients aged 25+ (84.5% said good). In fact, young patients were generally less positive across a range of different areas related to their experience at their GP practice compared with older patients.
For example, young patients were less likely to have a good overall experience of making an appointment (63.5%), compared with older patients (69.2%). They were also less likely to be aware of being able to book appointments through the online services offered by their GP practice (35.5%), compared with older patients (41.4%). In fact, young patients were less likely to be aware of other online services offered by their GP practice, compared with older patients. For example, those aged 16-24 were less likely to be aware of the ability to order repeat prescriptions online (30.5%) compared with older patients (38.9%), or accessing medical records online (11.0% compared with 13.0%).
In terms of mental health, young patients were more likely to say they had a mental health need at their last appointment (45.1% of 16 - 24 year olds compared with 40.8% of those aged 25+). Despite this, young patients were less likely to feel that the healthcare professional they last saw recognised and/or understood any mental health needs they had (83.8% compared with 87.5% of older patients).
There is growing awareness of the interrelationship between mental health and isolation (for example, Public Health England report that social isolation increases the risk of depression, and that depression in turn increases the risk of social isolation). It is therefore perhaps not surprising that young patients were also almost twice as likely to feel isolated from others, compared with older patients (11.0% compared with 6.1%).
While most young people do experience good health, one in three (31.2%) have at least one long-term condition. These young patients with long-term health conditions were less likely to feel positive about managing their health compared with older patients. For example, they were more likely to say they do not feel confident to manage any issues arising from this condition (23.6%), compared with older patients (15.5%). They were also more likely to say they needed support from local services or organisations (76.4%) to help them manage their condition(s), than older patients (69.2%). However, young patients were more likely to feel they did not receive enough support from local services (26.4% compared with 20.1% for older patients).
Meeting the communication needs of young people is an important aspect of care. The majority of young patients did feel that the healthcare professional they last saw or spoke to was good at listening to them (85.2%), but they were still less positive than older patients (89.2%).
Further analysis
GPPS provides a rich source of information on patient experiences of their GP practice. You can access and analyse the results by going to https://www.gp-patient.co.uk/ or email the team.
Technical note
Ipsos administers GPPS on behalf of NHS England. Approximately 2.2 million questionnaires were sent out nationally, and 758,165 were returned completed between January and March 2018. This represents a response rate of 34%. Data is weighted to match the profile of the population. Read further technical information about how the survey works here.
For more information about the survey, and to access the data see https://www.gp-patient.co.uk.