Cancer & Cardiovascular Disease: Lessons from COVID
 This article is not about how many people died from each disease; rather, it’s about the positive impact that could be made if we enacted the same approach to the two greatest killers, cancer and CV disease, as we’ve done with COVID-19.
This article is not about how many people died from each disease; rather, it’s about the positive impact that could be made if we enacted the same approach to the two greatest killers, cancer and CV disease, as we’ve done with COVID-19.
Drawing on data from Ipsos’ Global Oncology Monitor and other sources, Jackie Ilacqua considers how we could, and should, take learnings from the Covid-19 pandemic and apply them to other preventable, or at least treatable, diseases.
Cardiovascular (CV) disease and cancer kill more people every year than any other illness, including COVID-19. Looking at 2020, provisional CDC data show that the numbers of people in the United States who died from cardiovascular disease and cancer were 690,000 and 598,000, respectively. The number who died from COVID-19 was 345,000.
This article isn’t about how many people died from each disease. Rather, it’s about how many lives could be saved if we enacted the same approach to the two greatest killers, cancer and CV disease, as we’ve done with COVID-19.
Focusing specifically on cancer, imagine if you will a world where all people had free access to diagnostic testing and were expected to test every year for various types of very treatable cancers, like colorectal cancer. Take that one step further and think not only about access to testing but also information. A lot can be said, both positively and negatively, about the role that mainstream and social media have played in terms of information around COVID-19 – but never in my lifetime have I seen a ticker counting the number of cancer cases or the number of cardiovascular cases during daily news broadcasts. Counters showing the increasing prevalence of COVID-19, while frightening to many and perceived by others as overstated, demonstrated that COVID-19 was a real and serious threat. These tickers encouraged people to take symptoms seriously and adhere to measures to keep themselves safe.
Unsurprisingly, when Ipsos asked 20,000+ adults in 27 countries in late 2020 what they perceived to be the biggest health problem in their country, 72% of respondents said coronavirus/COVID-19; only 37% chose cancer and just 12% selected heart disease.
So, what’s the difference? Obviously COVID-19 is contagious while cancer and CV disease are not. Few countries have escaped the emotional and economic fallout of lockdowns and other restrictions. Moreover, the majority of people participating in Ipsos’ syndicated COVID-19 Consumer Therapeutics Study felt it was their social responsibility to get a COVID-19 vaccine, and that a top influencing factor in their decision-making was preventing transmission to others.
The concept of collective responsibility is not really applicable to cancer and CV disease and that is a key distinction – but the emotional and economic consequences of c.1.3m cancer/CV disease deaths every year, in the US alone, are enormous.
Returning to COVID-19, many states and countries mandated mask wearing and are now requiring proof of vaccination to enter restaurants or travel – yet cigarettes and other carcinogenic products are still legal. Think about that for just one second. Governments may have made efforts to stop the spread of secondary smoke with the ban on indoor smoking, but they are still allowing people to buy and smoke cigarettes freely even though smoking has been proven to cause cancer. US data from Ipsos’ syndicated Global Oncology Monitor show that 38% of the total reported patient sample between Aug 2020 – July 2021 were current or past smokers, with the highest rates recorded amongst lung and head & neck cancers.
When it comes to tackling cancer, early detection is certainly the best form of defense. According to the Mayo Clinic, 56% of people diagnosed with early-stage lung cancer live for at least 5 years after diagnosis. However, when diagnosed with late-stage lung cancer, the 5-year survival rate drops to just 5%. For people diagnosed in the later stages, the costs of treatment can be overwhelming to healthcare systems – and treatments are often not approved, or used at all, if the extension of life is not perceived to be long enough. To put some figures to this, an assessment of commercial claims data between 2009 - 2012 in the US put the average cost of treating a stage IV breast cancer patient (24 months post diagnosis) at $182,655, while the cost of treating a person diagnosed with stage I/II was $97,066. The difference is vast. The burden on the healthcare system is significant but, most importantly, the burden on the patient and their caregivers is enormous. Of course people are encouraged to get a colonoscopy, just as they were initially encouraged to get vaccinated or wear a mask, but certainly not as loudly, not as often, and not as passionately.
During the pandemic, I have heard multiple politicians say that even one death from COVID19 is too many – and I couldn’t agree more. But what about one cancer death? Conversely, during the height of the pandemic, many people delayed diagnostic testing while many cancer patients switched treatments to ones that required less frequent administration. Macmillan Cancer Support, a leading UK cancer charity, made the following estimates in its recent 2020 report, ‘The Forgotten ‘C’:
- Across the UK there are currently around 50,000 ‘missing diagnoses’ – meaning that compared to a similar timeframe last year, 50,000 fewer people have been diagnosed with cancer.
- Thousands fewer people in 2020 have started treatment after a cancer diagnosis than in 2019. In England alone, between March and August 2020, around 30,000 fewer people had started their first cancer treatment compared to the year before.
These findings are also reflected in Ipsos’ syndicated Global Oncology Monitor and COVID-19 HCP Impact Study data, from sampled physicians in the US. Across reported patient samples of breast, NSCL, CRC, prostate and gastric cancer cohorts, fewer newly diagnosed patients were reported by our participating physicians in the period Mar 2020 – Feb 2021 (‘during COVID’) than in Mar 2019 – Feb 2020 (‘pre-COVID’). See Figure 1.
Figure 1 – % reported cancer patients recorded as newly diagnosed ‘pre-’ vs ‘during COVID’ (US)
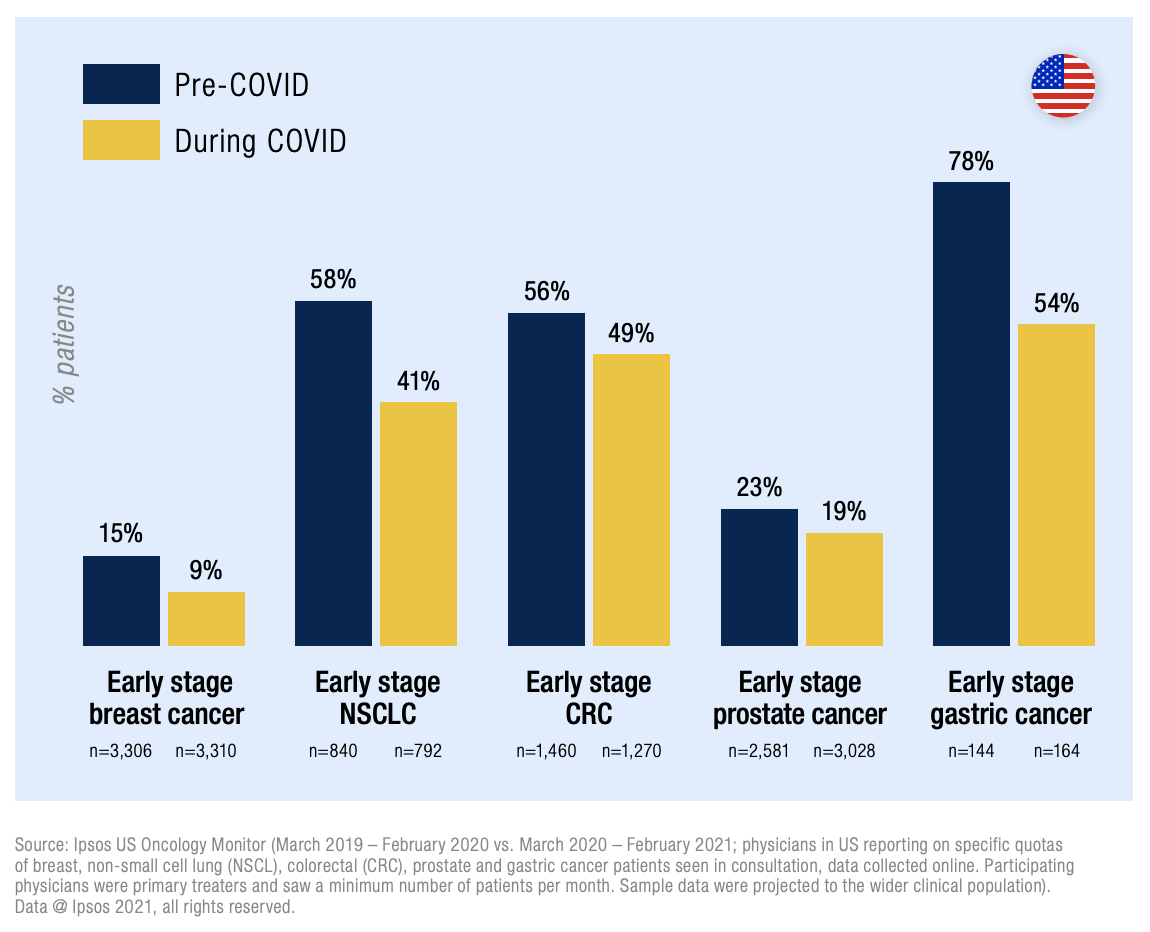 These data corroborate initial concerns expressed by sampled US physicians in our Oncology HCP COVID-19 Impact Study; during the fieldwork period of May 20 – June 1 2020, 23% of participants cited more notable/extreme delays in diagnosing cancer as a result of COVID-19. See Figure 2.
These data corroborate initial concerns expressed by sampled US physicians in our Oncology HCP COVID-19 Impact Study; during the fieldwork period of May 20 – June 1 2020, 23% of participants cited more notable/extreme delays in diagnosing cancer as a result of COVID-19. See Figure 2.
Figure 2 – % sampled physicians experiencing delays in diagnosing cancer as a result of COVID-19 (US)
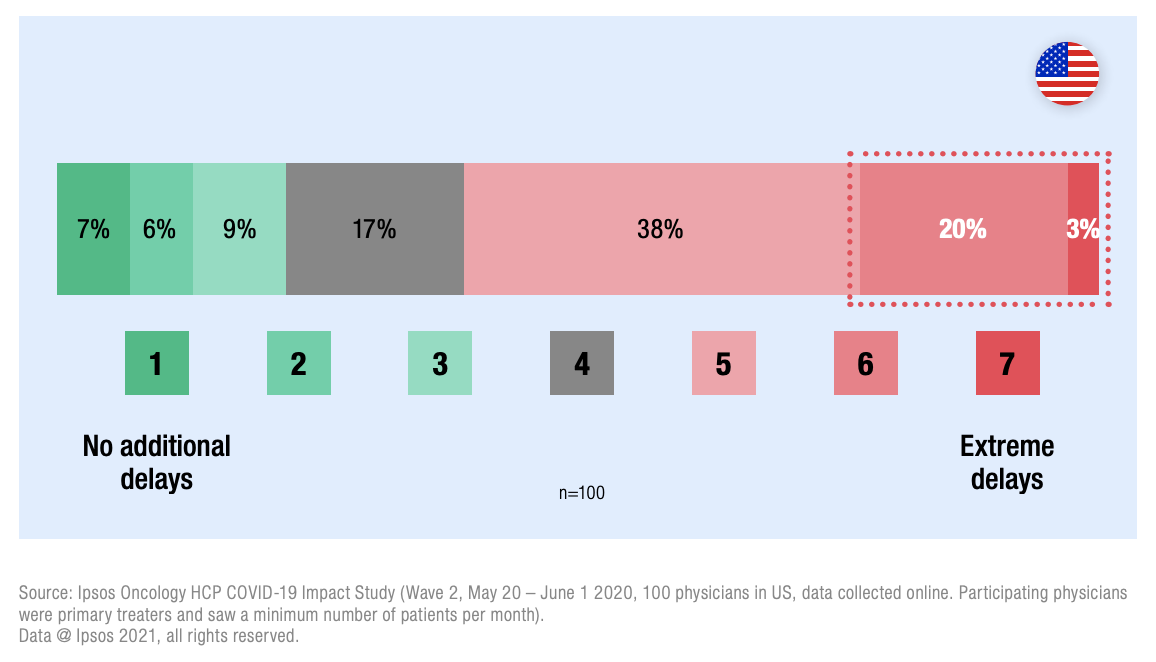 Alcohol is another primary risk factor for multiple cancers (including two of the most common types, breast and bowel cancer) and it is even less regulated than smoking. Alcohol and tobacco together have a cumulative effect, creating a higher risk of cell damage than either one alone – a fact that’s probably not as widely known as it should be. And that’s to say nothing of the widespread over-use of sugars and fats in the food that we buy. Being overweight can cause 13 different types of cancer, again including breast and bowel cancer, but the association between obesity and severe COVID-19 disease is far more widely known. Of course, this awareness-raising will have had positive impacts all round. Governments putting more efforts and resources towards preventing/tackling obesity will hopefully prevent countless deaths from all three types of disease. Indeed, Ipsos data show that, in Sept-Oct 2020, 45% of respondents in 30 countries claimed they were ‘trying to lose weight’.
Alcohol is another primary risk factor for multiple cancers (including two of the most common types, breast and bowel cancer) and it is even less regulated than smoking. Alcohol and tobacco together have a cumulative effect, creating a higher risk of cell damage than either one alone – a fact that’s probably not as widely known as it should be. And that’s to say nothing of the widespread over-use of sugars and fats in the food that we buy. Being overweight can cause 13 different types of cancer, again including breast and bowel cancer, but the association between obesity and severe COVID-19 disease is far more widely known. Of course, this awareness-raising will have had positive impacts all round. Governments putting more efforts and resources towards preventing/tackling obesity will hopefully prevent countless deaths from all three types of disease. Indeed, Ipsos data show that, in Sept-Oct 2020, 45% of respondents in 30 countries claimed they were ‘trying to lose weight’.
While it is unlikely that tobacco and alcohol will become illegal any time soon, governments, media companies and the healthcare community can do much more to help reduce the number of cancer and cardiovascular disease mortalities. We need to take the learnings from the COVID-19 pandemic and apply them to other preventable, or at least treatable, diseases. We already see pharmaceutical companies investing in and focusing on developing more vaccines, but early detection is the best way to avoid death in cancer and cardiovascular disease. Payers requiring annual physical exams, certain diagnostic tests, and a continuous media campaign showing the figures around these diseases and how the mortality rate decreases with early detection and intervention will save or prevent at least one death – which we already know is one too many.
All of this raises the specter of another lesson that COVID-19 has taught us: that the gap between rich and poor is vast and widening. Depending on the country we live in, disease prevention and treatment can be a very uneven playing field. By contrast, those of us who have been able to receive a COVID-19 vaccine probably had it for free. In some countries, COVID-19 PCR and rapid tests are free on request. This has undoubtedly had a huge impact on vaccination uptake and testing rates. So, while prevention and early detection are our main weapons in the fight against cancer and CV disease, we need to find a way to make consults and diagnostics more accessible for people of all incomes. Unfortunately, there are no easy answers here, but if COVID-19 has taught us anything it’s that when there’s a collective will and support, the medical community can achieve great things.

![[WEBINAR] Dealmaking 2026: What’s Changing, What’s Not, and How to Position for the Next Wave](/sites/default/files/styles/list_item_image/public/ct/event/2026-03/deal.png?itok=NtU1lGCc)

