“The NHS is broken but it’s not beaten”: Public opinion on A&E wait times
Healthcare is an issue that touches us all. In fact our data shows that it remains Britain’s primary worry, with two in five (40%) of us citing it as one of the issues we are most concerned about in the country (What Worries the World survey – Ipsos).
While our latest survey for the Health Foundation shows a trend of less negativity and more optimism across the NHS and social care, the latest findings highlight perceptions are still largely negative overall. A key priority for a third of the public (33%), which may come as no surprise, is improving NHS waiting times for A&E.
Public concern here reflects the fact that A&E waiting times have worsened in recent years. To put it in perspective, in the first quarter of 2014 around 150 people waited 12+ hours for admission. Fast forward to 2024, and that number has grown significantly to nearly 150,000 in the first quarter alone. It's a stark increase that highlights why this issue is at the forefront of people’s minds.
Concern also stems from staff within the healthcare system. A report by the Royal College of Nursing covering the experiences of NHS nursing staff revealed almost seven in ten (67%) are providing care in overcrowded and unsuitable places, such as corridors and converted cupboards daily.
Based on this, our latest poll tests the extent of public concern around A&E wait times, the availability of beds, and whether this affects behaviours for seeking care.
What do the public think about the NHS and access to care? Well, it’s complicated.
People appreciate the NHS but think there is room for improvement. On one hand, three in five (58%) Britons agree the NHS provides a high standard of care to patients. However, four in five (81%) say they are sad about the current state of the NHS, and seven in ten (71%) even say it makes them angry.
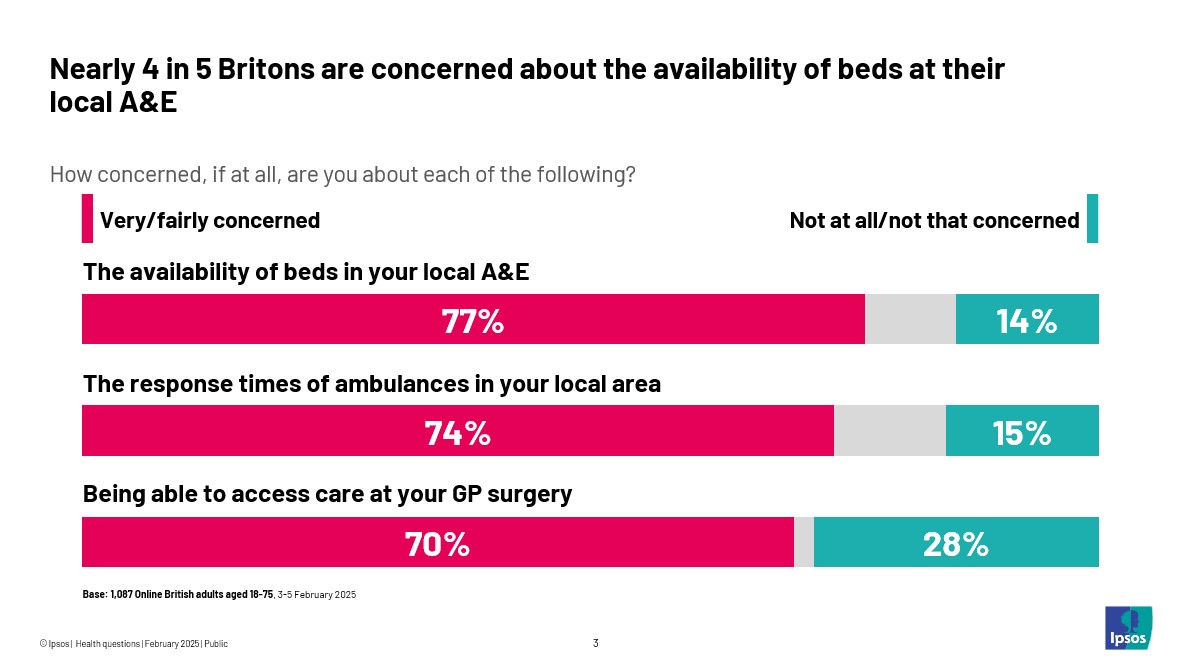
There is a real worry about having to wait for care, with over three quarters (77%) of people concerned about the availability of beds in their local A&E. Almost as many (74%) say they are concerned about the response times of ambulances, and seven in ten (70%) say they are concerned about being able to access care at their GP practice.
A key question that arises of course is whether these feelings about the NHS affect how people behave. For example, we found in polling we conducted in the last quarter of 2024 a concerning trend of people avoiding NHS services. As a result of anxieties about the NHS system, one third (33%) avoided A&E visits.
We can see a similar effect here. Worryingly, the data shows that this concern could impact behaviour. Two in five (40%) of those concerned about capacity at their local A&E say this makes them less likely to seek emergency care if they need it. Similarly, concern about ambulance response times also seems to have an effect. Of the 74% of Britons concerned about ambulance response times in their local area, nearly three in five (58%) would be more likely to seek alternative forms of transport to get to the hospital in an emergency.
Who is feeling more negatively about the current state of the NHS?
While levels of dismay about the NHS are high across the board, some groups appear more worried than others. Given that we have seen that concern could put people off from seeking care, it’s important to consider who is most concerned. We found that older people, those in social grades ABC1, and those of white ethnicity express higher levels of concern. For example, over nine in ten people aged 55 and over say they are sad about the current state of the NHS (91%), compared with seven in ten of those aged 18-34 (71%). Eight in ten people of white ethnicity say it makes them sad (83%) compared with two thirds of people from ethnic minority groups (66%). We see a similar sort of pattern in relation to concern about access but none of the findings are significant.
We also wanted to look at differential behaviour amongst those who are concerned but found little of significance. We have seen above that those in higher social grades are sadder, but amongst people who are concerned about the state of the NHS, are those in lower social grades more likely to put off seeking care? There’s little evidence of this in our data. It appears that concern influences behaviour in a similar way across demographic groups. Just one point of difference emerged – amongst people who told us they were concerned about the availability of beds in their local hospital, women were less likely to seek emergency care because of this (45% vs 34% men).
Overall...
It’s clear that the state of the NHS is very much a live topic for the public, with some groups more heightened to it. And this is important because it affects their behaviour, potentially dissuading them from seeking care early on. But at the same time, there is a still an affection for the NHS and a belief in the care provided by it. For example, when we asked the public Which of the following words, if any, do you most strongly think of when you think of the NHS? most said ‘long waiting times’ (57%), followed by ‘understaffed’ (51%). However, around a quarter (24%) said ‘high quality of care’. This is the best way to sum up the complex relationship the British public have with the NHS. It is undoubtedly facing challenges, and these challenges are reflected in the public's perception and behaviour. While there is a glimmer of optimism, the underlying concerns about access to care, particularly in emergency situations, are undeniable. Understanding these concerns, and how they differently impact various demographics, is crucial for creating a healthcare system that truly serves everyone.





